This really sucks
How I learned to love my wound vac
I’ve entered a new phase with my leg wound treatment.
But first a health roundup.
Physical therapy is critical to my healing. I’m walking mainly without the cane, even in the garden. "I’m using the hose as an assistive device,” I said to my physical therapist. Raised eyebrows was her response.
Wound therapy is progressing. More below.
Ulcerative colitis (UC) continues to plague me. I had a sigmoidoscopy in August. During the procedure — I was awake for it! — the tissue appeared less inflamed. Biopsy results revealed good news — there was nothing like colon cancer. And bad news — I still have UC. I will start a new drug treatment soon.
I will visit the oncologist for next steps soon.
I have a new chronic condition: lymphadema. My first lymphadema therapy takes place today.
The Wound: Terrifingly beautiful
As I introduced in the “What is a weekend” post, eschar at the infection site has limited my motion, causing pain and preventing me from healing. Scroll down to The fascinating world of wound care to read more about eschar.
I thought it couldn’t get any worse but learned that it was just the beginning.
In late July, the surgeon debrided the eschar and placed the first wound vac. The surgery had enlarged the carveout on my leg to yield a wound area of 22.5 x 17.8 cm (8 x 7 in). The wound wraps around the sides and back of my right calf.
That the pseudomonas bacteria did this damage in a matter of hours on July 9 still leaves me speechless. As much as I hate that this happened to me, I have to respect the bacteria.
Necrotic tissue that won’t quit
Eschar is necrotic tissue that impedes healing and can cause infection. Skin heals best in an orderly fashion, unobstructed by necrotic tissue. Adipose tissue in the wound bed also falls in this category of necrotic tissue as it forms scar tissue that the body must work around as it rebuilds the skin. The adipose tissue had to go.
Enter the wound clinic.
My three weekly visits include one session with the wound surgeon, who scrapes away the offensive tissue. The goal is to create an environment favorable for healing, as evidenced by granulation tissue formation (red tissue). As you might suspect, this is not fun and progress was slow at first. Then over one weekend, viable tissue increased from 5% to 20%. It’s now close to 90%.
How could this be?
Complementary interventions
The surgeon’s debriding complemented the constant work of the wound vac and resulted in better results than if only one therapy was used.
The wound vac is a system that uses negative pressure to draw drainage away from the wound. A nurse applies a special dressing to the wound, and a small device connects the wound through tubing to a canister that collects the drainage.
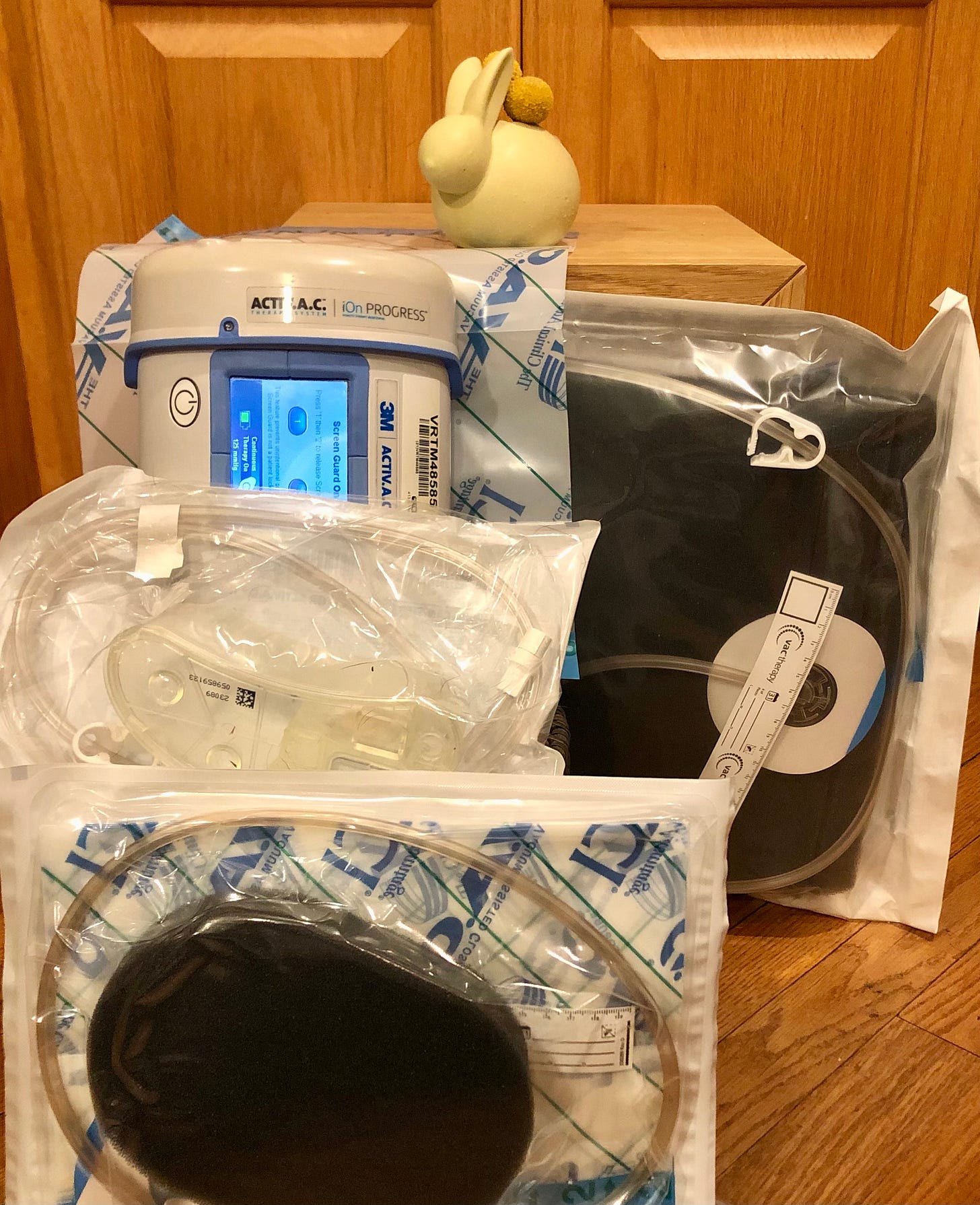
The nurse cuts the dressing to size, places the vac tube connector on the dressing, and covers the area in closure film to prevent leaks. Finally, the nurse turns on the vac, which causes the dressing to shrink into place.
I need to “wear” the vac 24/7.
Wound care supplies are abundant. I use only tape, closure film, and gauze at home.
The vac is an inanimate object
It’s taken me awhile to appreciate the wound vac. In fact, I’ve been downright angry with it for ruining my life. I could often be heard to say: “This Sucks! I hate it!”
I would get mad at the vac every time I set it down upright — precariously — and it would tip over. Or when I would forget that I was attached to the thing after setting it on the couch and then trying to walk away.
One might say that I didn’t want to accept my situation. That I preferred to stay mad.
Today I appreciate the device and even say so as I pick it up to carry it with me. It’s improving my life. How could I not appreciate it? “This Sucks So Well!”
More important, I am no longer looking away from my situation. Nor am I devastated. I’ve accepted that this is my reality.
Viable tissue has nerve endings
Of course, treatment brings change. As more viable tissue appears, nerve endings are available to fire, too. As a result, the sessions at the wound clinic and afterwards are more painful.
A supposition is that this pain is disorganized. Gabapentin can help by calming neural pathways, and I’ve started taking the drug, which has helped some.
Return to the present
What helps me the most is returning to the present moment. As often as I can, I breathe in and out, with a focus on now. Not what’s happened in the past. Not what might take place in the future.
I use breathing often during medical procedures. I also want to learn to stop and pause during every day moments of frantic busyness or to mark the transition from one phase in the day to another, e.g., late afternoon as I close down work projects and ready myself for the evening.
When I do pause, it’s always worth it.





Wow. Just wow. You continue to amaze me with all that you are going through and how you are handling it. To be able to "love" your wound vac sounds crazy until you put it into context of what it does and how it is helping you to heal. Sending you all the good vibes I can and praying that you will continue to heal more each day. Love you Leah!
You are a true inspiration to me. I admire your honesty, your attitude, and your tenacity.